
Foot Hyperpronation

Get to the Foundation of Your Patient’s Problem
Healthcare is changing- and regardless of who is ultimately paying for your care, they want results. Now, more than ever, you must recognize the “functional” diagnoses that contribute to your patient’s “structural” problems. This article will discuss the identification and successful management of Foot Hyperpronation- a commonly overlooked “functional” problem that delays recovery.
The foot and ankle combination is a complex tool that is called upon to perform two seemingly contrary roles; a flexible shock absorber that contours to irregular surfaces, and a rigid propulsive lever. “Pronation” plays a vital role in the foot’s ability to multitask. (1,2,3)
Foot pronation is the combined movement of eversion, abduction, and dorsiflexion that results in flattening of the longitudinal arch. (4) In a normal gait cycle, the process of pronation begins at heel strike, progresses through mid-stance and then reverts back toward supination to prepare a rigid lever for forward propulsion. (4-7) In a healthy foot, pronation is limited to approximately 8 degrees. (5-7) Movement beyond 8 degrees is termed “hyperpronation.”
Since the longitudinal axis of the tibia is medial to the body of the calcaneus, loading this joint forces the heel laterally in relation to the tibia (calcaneal eversion). As the center of gravity moves medially, the foot may compensate by rotating laterally, making it a poor lever. The repetitive stress of hyperpronation causes significant strain on the soft tissues of the foot. The relatively inelastic medial band of the plantar fascia is often stressed beyond its capacity to elongate, causing irritation in those who hyperpronate. (10) Traction from hyperpronation contributes to posterior tibial tendinopathy and posterior tibial nerve irritation (tarsal tunnel syndrome). (11)
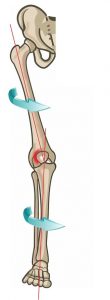
The effects of hyperpronation are not localized to the foot. Due to the unique shape and tight fit of the ankle mortise, hyperpronation causes internal rotation of the tibia. (12) This torque continues up the kinetic chain and results in internal rotation of the femur, which moves the femoral head and acetabulum backward, causing anterior tilt of the pelvis, and hyperextension of the lumbar spine (see figure 1). (7,8,14,15)
Hyperpronation stresses the knee through a number of mechanisms. In particular, a lowered arch combined with internal tibial rotation places significant valgus stress on the knee. (8) This challenges the medial collateral ligament and anterior cruciate ligament and is a well-recognized contributor to injuries of these structures. (16,17) Additionally, internal rotation of the tibia and femur cause a relative lateral displacement of the patella, driving the lateral patellar facet into the lateral femoral condyle. (18) Not surprisingly, low arches and hyperpronation are commonly associated with patellofemoral pain. (19-22) Longstanding misalignment of the patellofemoral joint is associated with degeneration. (19,22,23)
Not all of the torsional energy of tibial internal rotation is dissipated by the knee. In fact, much of it travels through the knee into the thigh and is absorbed by the hip. (18) Internal rotation of the femur has a detrimental effect on several muscle groups, including the quadriceps, hip adductors, and hip abductors (gluteus medius). (8) Foot hyperpronation and hip abductor weakness are known biomechanical coconspirators- hyperpronation causes stretch weakness of the gluteus medius, and gluteus medius weakness allows excessive hip adduction which causes increased foot arch loading during ambulation. So in a self-perpetuating cycle, the compensatory changes that occur upstream in response to hyperpronation serve to exacerbate problems at the foundation.
Internal rotation of the femur causes the pelvis to shift anteriorly. (8) This further contributes to “stretch weakening” of the gluteal and abdominal muscles and adaptive tightening of the hip flexors (lower crossed syndrome). This process limits hip extension, which in turn increases extension forces on the lumbar spine facets. (8) What’s more, the functional leg length inequality of a unilateral flat foot may cause lateral bending of the lumbar spine toward the affected side, further increasing facet compression. (8) As expected, hyperpronation contributes to lower back pain. (14,25-32)
Foot hyperpronation and pes planus and are distinctly separate problems, with the former being “dynamic” and the latter “static.” However, the two are related and the negative effects of hyperpronation may be compounded in low-arched patients.
The body employs various compensatory mechanisms to offset foot hyperpronation – although these corrections do not come without a cost. (8) Foot hyperpronation ultimately causes joints higher in the kinetic chain to absorb more shock. (8,20,21,30) The increased load on the knees, hip, and spine is compounded during athletic activity, particularly running and jumping. While the “functional” diagnosis of foot hyperpronation can present asymptomatically, it is a well-known contributor to a multitude of painful “structural” diagnoses throughout the lower body.
There is no “typical” presentation for foot hyperpronation, but the condition should be considered in any patient with lower chain symptomatology, particularly those with plantar fasciitis, Achilles tendinopathy, metatarsalgia, medial tibial stress syndrome (shin splints), patellofemoral pain syndrome, greater trochanteric pain syndrome, and low back pain. Longstanding hyperpronation may lead to ligamentous laxity and degeneration of affected joints. (19-23,39,40)
Clinical evaluation for foot hyperpronation begins with visual inspection of a barefoot patient. (41) Ideally, a sagittal plane projecting forward from the axis of the tibia should also pass through the second ray of the foot. Patients with hyperpronation commonly demonstrate excessive forefoot abduction. This may be assessed by observing the degree of foot abduction from behind- aka “too many toes sign.” Visual inspection of the posterior ankle will often demonstrate calcaneal eversion, as evidenced by inward “bowing” of the Achilles tendon. Sliding a finger beneath a standing patient’s medial longitudinal arch may provide a simple assessment of static arch height.
As noted earlier, hyperpronation is a functional problem (not simply “flat feet”), so it must be assessed functionally. The navicular drop test is a useful functional measurement. The test begins with marking the position of the seated patient’s navicular by placing a dot over their navicular tuberosity, while their foot is in a non-weight bearing and neutral position. The clinician then places an index card on the floor next to the patient’s foot and marks the index card at the position of the dot. The patient then stands (on both feet), and the clinician marks the new position on the card. If the navicular drops more than 10 mm, the test is positive for hyperpronation. (42,43) Normal navicular drop is 6 to 8 mm. (42)
Posterior tibialis weakness is another possible contributor to foot hyperpronation. Weakness of this muscle is suggested by excessive calcaneal eversion when performing a heel raise. Muscular assessment should include evaluation of hip abductor strength via the Trendelenberg sign or knee valgosity on single leg squat or single leg step up. Since the Achilles tendon inserts slightly lateral to midline, a hypertonic gastroc/soleus will result in some degree of calcaneal eversion and increased pronation. Clinicians should assess flexibility of the gastroc and soleus in passive ankle dorsiflexion.
The management of foot hyperpronation includes prescribing arch supports as well as exercises to control motion at the hip and ankle. (35) Factors, including the degree of hyperpronation and the functional demands of the patient, will dictate whether custom or prefabricated orthotics are most appropriate. Clinicians should be cautious to avoid excessive arch buttressing, as this could produce a paradoxical result. (47) Likewise, bulky orthotics or shoes with excessive cushioning may have an adverse effect on proprioception and balance. (47)
Inadequate ankle dorsiflexion may force excessive pronation through the mid foot. Stretching exercises and myofascial release may be appropriate for restrictions in the gastroc and soleus muscles.
Strengthening exercises should be directed at the foot and hip, specifically the posterior tibialis and hip abductor muscles. Traditional strength training does not necessarily change faulty movement patterns. (54) Exercise programs should incorporate proprioception, beginning with simple balance training like a single leg stance or Vele’s, then progressing to lunges on an unstable surface, like a Bosu or Dynadisc. (55-57) Strengthening exercises for the hip abductors could include a posterior lunge, clam with band, or sidebridge.
Obesity exacerbates hyperpronation; therefore, diet and exercise recommendations may be appropriate for overweight patients. (64,65) Hyperpronators should avoid shoes with narrow toe boxes or high heels. (11) Of note- hyperpronation is common in children, as the development of the longitudinal arch is usually not complete until the age of 8. (41) Some studies suggest that shoe wear in children is detrimental to the development of a healthy longitudinal arch. (62,63)
References
- Waerlop I, Allen S. Pedographs and Gait Analysis: Case Studies and Clinical Pearls. Victoria, BC, Canada: Trafford, 2006.
- Michaud T. Foot Orthoses and Other Forms of Conservative Foot Care. Newton Mass.: Michaud, 1993:29.
- Phillips RD, Phillips RL. Quantative analysis of the locking mechanism of the midtarsal joint. J Am Pod Med Assoc, 1983;73:518-22.
- Minkowsky R. The spine, an integral part of the lower extremity. In: Clinical Biomechanics of the Lower Extremities, Valmassey R. St Louis: Mosby, 1996:105.
- Close JR, Inman VT, Poor PM, Todd FN. The function of the subtalar joint. Clin Orthop, 1967;50(1-2):159-79.
- Wright DG, Desai SM, Henderson WH. Action of the subtalar and ankle joint complex during the stance phase of walking. J Bone Joint Surg, 1964;46A(2):361-82.
- Perry J. Gait Analysis: Normal and Pathological Function. Thorofare, NJ: Slack, 1992:73.
- Manter JT. Movements of the subtalar and transverse tarsal joints. Anat Rec 1941;80(4):397-409.
- Stovitz SD, Coetzee JC. Hyperpronation and Foot Pain. The Physician and Sportsmedicine- Vol. 32 – No. 8 – August 2004
- Mann RA, Baxter DE, Lutter LD. Running symposium. Foot Ankle, 1981;1(4):190-224.
- Cibulka MT. Low back pain and its relation to the hip and foot. J Orthop Sports Phys Ther, October 1999;29(10):595-601.
- Michaud T. Foot Orthoses and Other Forms of Conservative Foot Care. Newton, Mass.: Michaud, 1993;59-62.
- McLean SG, Huang X, Su A, Van Den Bogert AJ. Sagittal plane biomechanics cannot injure the ACL during sidestep cutting. Clin Biomech 2004;19(8):828-838.
- Loudon JK, Jenkins W, Loudon KL. The relationship between static posture and ACL injuries in female athletes. J Orthop Sports Phys Ther 1996;24(2):91-97.
- Lafortune MA, Cavanagh PR, Sommer HJ, Kalenak A. Foot inversion-eversion and knee kinematics during walking. J Orthop Res 1994;12(3):412-420.
- Klingman RE. Foot pronation and patellofemoral joint function. J Orthop Sports Phys Ther, 1999;29(7):421.
- Zammit GV, Payne CB. Relationship between positive clinical outcomes of foot orthotic treatment and changes in rearfoot kinematics. J Am Podiatr Med Assoc, May – June 2007;97(3):207-12.
- Root RC, Orien WP, Weed JH. Normal and abnormal function of the foot. Clinical Biomechanics, 1977.
- Rothbart BA, Estabrook L. Excessive pronation: a major biomechanical determinant in the development of chondromalacia and pelvic lists. J Manipulative Physiol Ther, 1988;11(5):373-9.
- Ross FD. The relationship of abnormal foot pronation to hallux abducto valgus – a pilot study. Prosthet Orthot Int, August 1986;10(2):72-8.
- Michaud T. Foot orthoses and other forms of conservative foot care. 2nd ed: Thomas Michaud; 1997. p 56-70, 89, 114-17
- Dananberg HJ, Guiliano M. Chronic low-back pain and its response to custom-made foot orthoses. J Am Podiatr Med Assoc 1999;89:109-17
- Larsen K, Weidich F, Leboeuf-Yde C. Can custom-made biomechanic shoe orthoses prevent problems in the back and lower extremities? A randomized, controlled intervention trial of 146 military conscripts. J Manipulative Physiol Ther 2002; 25:326-31.
- Cibulka MT. Low back pain and its relation to the hip and foot. J Orthop Sports Phys Ther, October 1999;29(10):595-601.
- Waerlop I, Allen S. Pedographs and Gait Analysis: Case Studies and Clinical Pearls. Victoria, BC, Canada: Trafford, 2006.
- Botte RR. An interpretation of the pronation syndrome and foot types of patients with low back pain. J Am Podiatr Med Assoc, May 1981;71(5):243-53.
- Root RC, Orien WP, Weed JH. Normal and abnormal function of the foot. Clinical Biomechanics, 1977.
- Michaud TC. Development of the Arch: Functioal Implications. Lower Extremity Review.July 2012. http://lermagazine.com/article/development-of-the-arch-functional-implications . Accessed 11/28/14
- Allen S, Waerlop IF, Lardner R. A Few Words About Pronation Dynamic Chiropractic – February 26, 2008, Vol. 26, Issue 05
- Woodford-Rogers B, Cyphert L, Denegar CR. Risk factors for anterior cruciate ligament injury in high school and college athletes. J Athl Train, 1994;29(4):343-6.
- Krivickas LS. Anatomical factors associated with overuse sports injuries. Sports Med, 1997;24(2):132-46.
- Gould N, Moreland M, Alvarez R, et al. Development of the child’s arch. Foot Ankle 1989;9(5):241-245.
- Shrader JA, Popovich JM, Gracey GC, Danoff JV. Navicular drop measurement in people with rheumatoid arthritis: interrater and intrarater reliability. Phys Ther 2005;85:656-64.
- Brantingham JW, Gilbert J, Shaik J, Globe G. Sagittal plane blockage of the foot, ankle and hallux and foot alignment— prevalence and association with low back pain. J Chiropr Med 2006;5:123-7.
- Robbins SE, Hanna AM. Running-related injury prevention through barefoot adaptations. Med Sci Sports Exerc. 1987;19:148-156.
- Willy R, Davis I. The effect of a hip-strengthening program on mechanics during running and during a single-leg squat. J Orthop Sports Phys Ther 2011;41(9):625-632.
- Rotem-Lehrer N, Laufer Y. Effect of focus of attention on transfer of a postural control task following an ankle sprain. J Orthop Sports Phys Ther. 2007;37:564-569.
- McNevin NH, Wulf G. Attentional focus on suprapostural tasks affects postural control. Hum Mov Sci. 2002;21:187-202.
- McNevin N, Wulf G, Carlson C. Effects of attentional focus, self-control, and dyad training on motor learning: implications for physical rehabilitation. Phys Ther. 2000;80:373-385.
- Rao UB, Joseph B: The influence of footwear on the prevalence of flat foot: a survey of 2300 children. J Bone Joint Surg Br 1992;74(4):525-527
- Messier SP, Davies AB, Moore DT, et al: Severe obesity: effects on foot mechanics during walking. Foot Ankle Int 1994;15(1):29-34
- Hills AP, Hennig EM, McDonald M, et al: Plantar pressure differences between obese and non-obese adults: a biomechanical analysis. Int J Obes Relat Metab Disord 2001;25 (11):1674-1679
- Williams DS, McClay IS, Hamill J. Arch structure and injury patterns in runners. Clin Biomech 2001;16(4):341-347.



















