
Calcification of the Stylohyoid Ligaments and Thyroid Cartilage Mimicking Vertebral Artery Calcification

Calcification of the stylohyoid ligaments or thyroid cartilage may be frequently mistaken for calcific plaquing of the vertebral artery. In actuality, calcification of the vertebral arteries is extremely rare. The calcification of the stylohyoid ligaments and thyroid cartilage is commonly encountered and should not be mistaken for arterial calcification. If both the APLC and lateral cervical views are compared, this mistake should virtually never happen. Although on the APLC view the calcifications may appear to be in the general area of the vertebral arteries, correlation of the calcifications with the lateral projection should quickly dispel this impression.
Eagle Syndrome
With stylohyoid ligament calcification, the lateral view readily demonstrates that the calcification is proceeding from the styloid process and continues inferiorly at an angle toward the hyoid bone (fig. 1). In vertebral artery calcifications, the calcification would be more vertically oriented and correspond to their course through the foramen in the cervical transverse processes. Stylohyoid ligament calcification may not be without symptoms, however. Although uncommon (less than 4% of the population show calcification and a smaller percentage experience symptoms), these symptoms are termed “Eagle syndrome” and are the result of compression of adjacent nerves or blood vessels (1). Symptoms are more common in women. They may include difficulty swallowing, a sensation of something stuck in the pharynx, shooting pains from the throat to the ear, pain at the base of the tongue, pain when turning the head, tinnitus or buzzing in the ears, headaches, or throbbing in the mandible. Diagnosis rests with an x-ray image showing elongation of the styloid process with possible calcification of the stylohyoid ligament. The calcification may be extensive and appear to be jointed (fig. 2). Treatment for Eagle syndrome ranges from surgery to steroid injections. Conservative care, consisting of manipulation and physiotherapy, may provide relief as well.
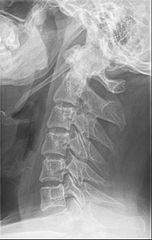
Figure 1 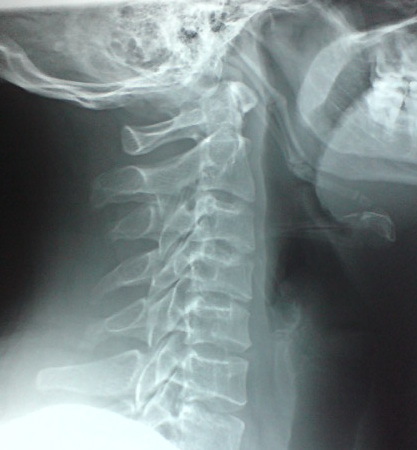
Figure 2
Thyroid Cartilage Calcification
Another radiographic finding that
has been confused in some cases with vertebral artery calcification is
calcification of the thyroid cartilage. On the APLC view, this may appear as parallel
lines of calcification overlying the articular pillars of the cervical spine (fig.
3). If the calcifications actually resided in the vertebral arteries, these
lines would be positioned farther laterally over the transverse processes. A quick
comparison with the lateral view (fig. 4) will reveal mottled calcification
beneath the hyoid bone, which corresponds to the thyroid cartilage. Thyroid
cartilage calcification is asymptomatic and does not imply pathology of the thyroid.
The main point is to recognize the finding for what it is, and not to confuse
it with arterial calcification. Thyroid cartilage calcification (and subsequent
ossification) usually begins after adolescence (2) (although there have been rare
cases that have occurred during adolescence), and gradually increases with age.
The exact mechanism for calcification is not well understood. The extent of
calcification tends to be less in women, and they seldom show complete
ossification. It has been proposed that a hormonal influence may exist. The calcification
often begins at the posterior margin of the thyroid cartilage lamina. The
degree of calcification may not be symmetrical; however, it tends to be bilateral.
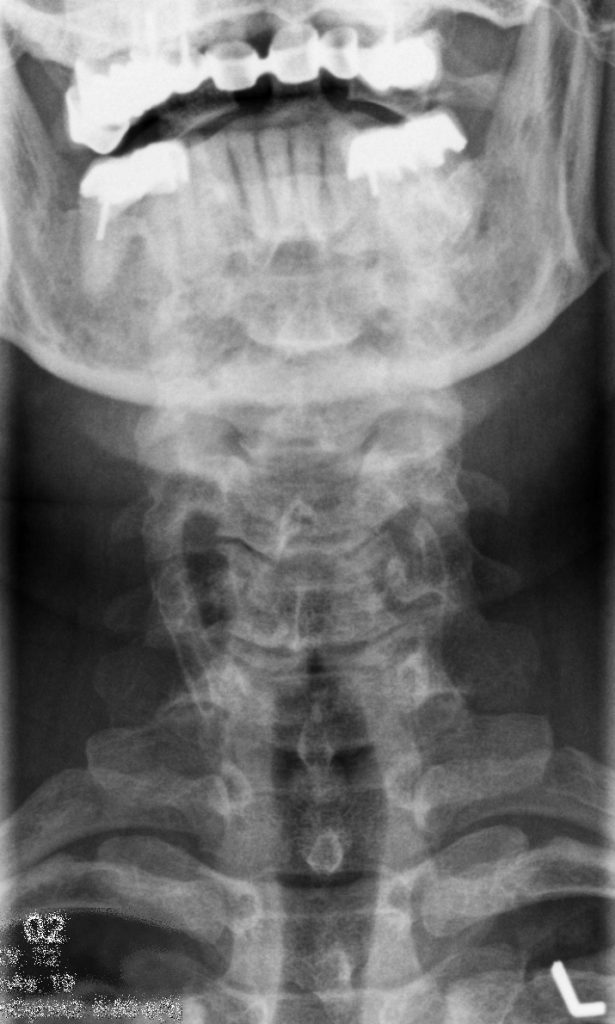
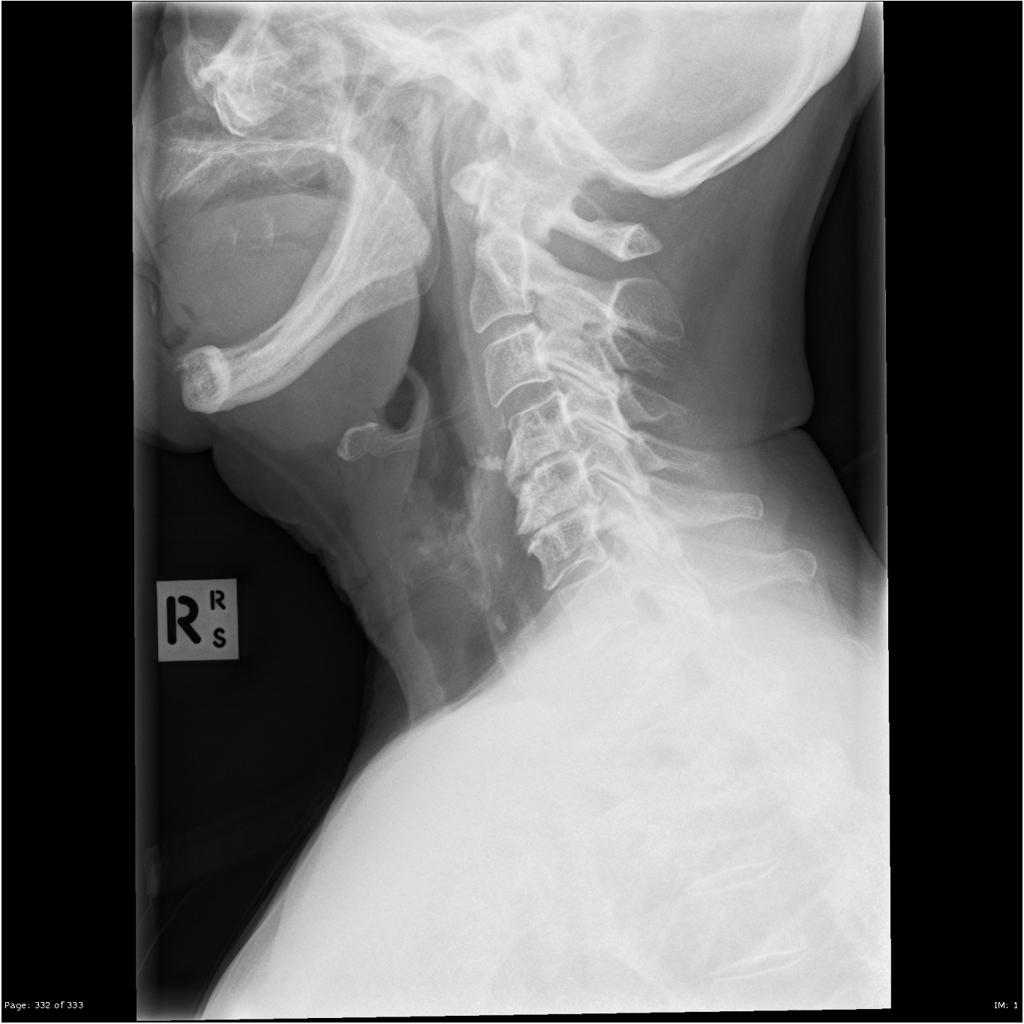
In conclusion, it is fairly easy to differentiate stylohyoid ligament calcifications and thyroid cartilage calcifications, provided that both the lateral and AP cervical views are evaluated. Neither of these two diagnoses should be confused with vertebral artery calcification.
References:
1. Villines Z., Murall D.: “Medical News Today” Tuesday 29, May 2018.
2. Schultz N. T.: “Trends in Patterns of Ossification of Thyroid Cartilage” Trace: Tennessee Research and Creative Exchange.



















